Can Varicose Veins Cause Leg Cramps?
Leg cramps are sudden muscle contractions in the leg, typically around the calf or thigh, that cause pain and discomfort for short periods of time. Patients who get leg cramps often, especially at the end of the day, may be suffering from venous disease. Chronic leg cramps coupled with itching legs, leg tiredness, leg swelling, leg heaviness, a leg rash , skin discoloration, a skin ulcer, and restless leg syndrome may be a sign of a vein condition.
Can Varicose Veins Cause Leg Cramps?


What Causes Leg Cramps to Develop from Varicose Veins?

What Causes Leg Cramps to Develop from Varicose Veins?
Leg cramps associated with varicose veins are typically a result of poor blood circulation. Varicose veins occur when the vein valves are weakened or damaged, leading to blood pooling and increased pressure in the affected veins. This elevated pressure can contribute to muscle cramps and discomfort in the legs.
What are Other Symptoms of Venous Disease or Varicose Veins?

A feeling of heaviness or fatigue
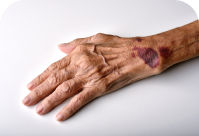
Skin discoloration

Restlessness

Leg cramping

Swollen legs or ankles

Relief from pain when legs are elevated

Burning veins in legs
What Treatments are Available for Leg Cramping?
There are Many Treatments for Leg Cramps Caused by Varicose Veins Available at StrideCare Including:

Diagnostic Arterial Ultrasound
A non-invasive test that uses ultrasound technology to get a full view of the arteries.

Radiofrequency Ablation
A small catheter emits radio waves into affected veins, cutting off blood flow.
Varithena™ Microfoam Ablation
Treats both varicose and spider veins using a concentrated, injectable foam
StrideCare
Patient Reviews



4.89 Average Online Review Score












StrideCare Leverages athenaOne to Enhance Financial and Operational Results, Improve Clinical Workflows
2 Min Read CASE STUDY: Transitioning all practices onto one united system gives StrideCare invaluable access to data
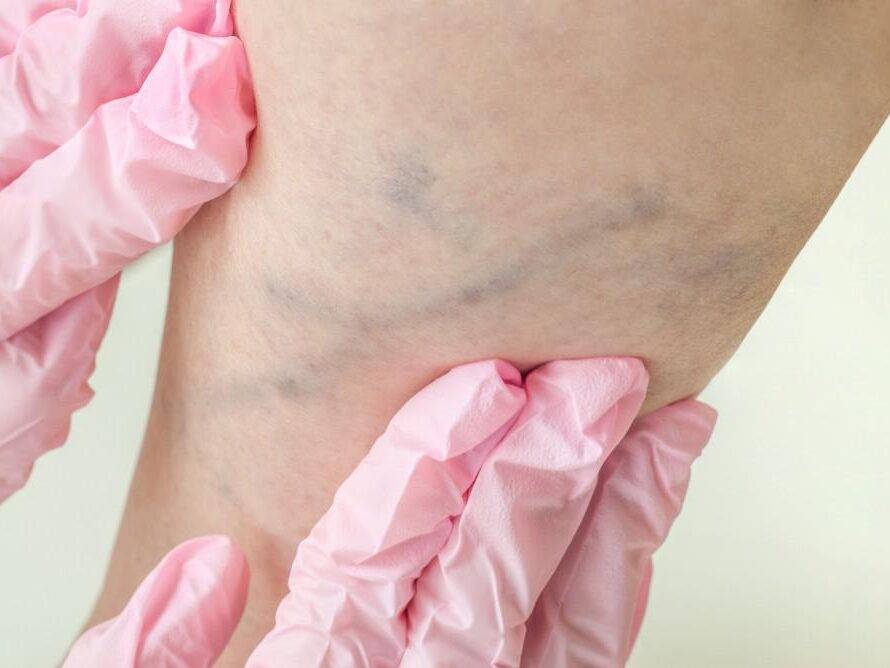
When are Varicose Veins More than Just a Cosmetic Concern?
2 Min Read Learn about varicose veins, prevention tips, and treatment options from StrideCare’s vein specialists in Texas.
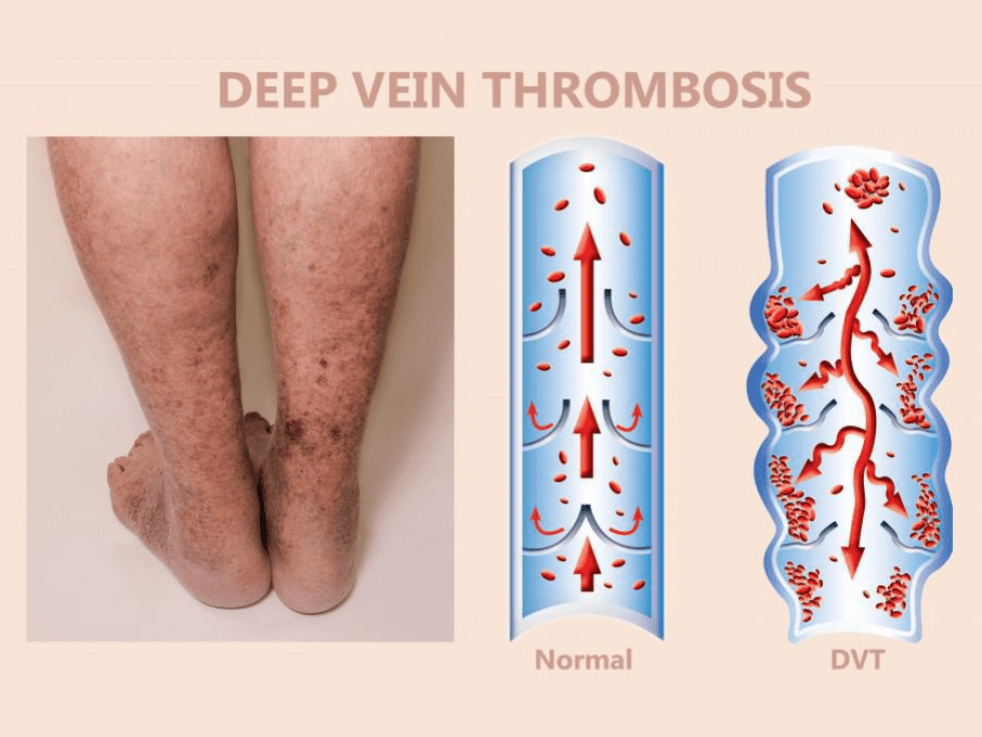
Puffy Legs are One of the First Signs of Deep Vein Thrombosis
3 Min Read Learn the symptoms of deep vein thrombosis (DVT) and seek immediate evaluation at StrideCare for expert care and treatment.