
What is Venous and Vein Disease?
Vein disease, also called venous disease, can develop over months or years from malfunctioning vein valves in legs. Normally functioning valves prevent backflow of blood down the legs and keep blood moving towards the heart. In a patient with vein disease, broken valves do not hold a seal and blood pressure builds up in the lower legs, leading to pooling blood called venous stasis. This results in leg swelling and skin changes.
 Request a vein disease consultation today if you are experiencing any of the following symptoms:
Request a vein disease consultation today if you are experiencing any of the following symptoms:
- Pain in the legs, including cramping and aching
- Darkening of the skin around the lower legs, ankles and feet
- Thick skin on the lower legs and ankles
- Swelling of the legs, restless legs
- Varicose and spider veins on the legs
- Chronic pelvic pain
Our Leg Vein Experts Can Help!
832-886-0137
CONSULTATION TODAY!
The later vein disease is detected, the harder it can be to treat. Luckily, since venous disease can be a slowly progressing chronic condition, later symptoms can be avoided with immediate screening and treatment. If you notice these symptoms, contact us today for expert evaluation and management of your vein disease.
Before & After Photos
Hamilton Vascular is your premier center for vein and venous disease treatment. Our results speak for themselves.



What Causes Chronic Vein Disease?
Anything that can physically damage vein valves can lead to chronic vein disease. Two common causes are deep vein thrombosis and superficial venous thrombosis. These are both conditions where blood clots form in veins. Once the clot dissolves, they leave scar tissue and permanent damage on the valves, preventing them from opening and closing properly. Also, some patients are predisposed to malfunctioning valves due to genetics and family history, such as a parent or grandparent with varicose veins. Women with multiple pregnancies are at a higher risk of developing chronic venous disease.
Pelvic tumors and vascular malformations, leading to abnormal flow of blood and pressure gradients in the vasculature, can lead to chronic vein disease. Additionally, chronic venous disease is associated with being overweight. Finally, weakness in leg muscles that squeeze blood back to the heart can also contribute to the development of vein disease.
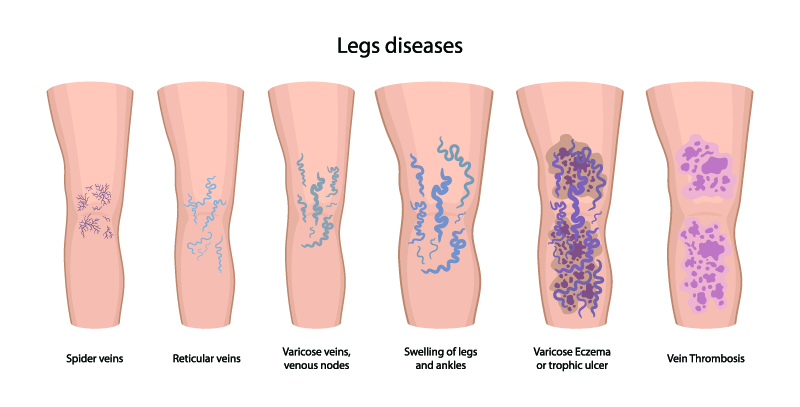
What Are Venous Disease Symptoms?
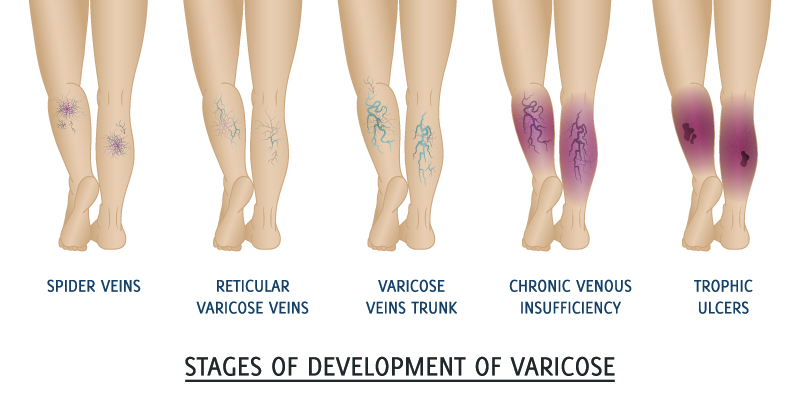
Chronic vein disease begins with small varicose veins, and can gradually progress to larger veins. As new veins develop and symptoms worsen, legs may experience swelling. This tends to occur more with long periods of standing or sitting. The swelling, when present for long periods of time, can lead to iron (hemosiderin) deposition in the skin known as lipodermatosclerosis. Later in the disease process, leg ulcers develop that require additional medical treatment to heal.
Symptoms of Chronic Venous Disease include:
- Swelling of the legs or ankles (edema)
- Pain that worsens with prolonged sitting or standing
- Pain that improves with leg elevation
- Pain when walking that relieves with rest
- Cramping of the legs
- Throbbing sensation in the legs
- Achy feeling in legs
- Heaviness feeling in the legs
- Itchy skin and sensation in the legs
- Thickening of the skin with “woody” changes
- Skin around the ankles changing colors to red or brown
- Wounds on the lower legs that do not heal, usually around and above the ankles
- Newly formed varicose veins
- Abnormally flaky skin, or abnormally moist skin
- Tightness in the calves
Meet Our Expert Doctors

Dean Chauvin, MD

Carlos Hamilton III, MD

Andrew Hansen, MD

Mary Parker, MD

William Parker, MD

Terrell Singleton, MD

Justin Smith, MD
How Is Chronic Vein Disease Treated?
The first step in treating venous disease is to reduce to pressure in the veins. Our experienced physicians will recommend treatment options based on the cause of your leg condition, your health status, and your history. Other factors we consider are:
- Onset, duration, timing, exacerbating and relieving factors of your symptoms
- Your age
- Severity of your condition
- Presence of ulcers and skin changes
- Your past history of blood clots and DVT
- Your ability to tolerate medications and procedures
Initial chronic vein disease treatment usually includes compression stockings, leg elevation, exercise, weight loss, moisturizing the skin to prevent cracks, and prescription medications. Many patients benefit from venous closure using radio frequency ablation and ultrasound guided percutaneous sclerotherapy.
In serious cases, venous closure may needed immediately, for instance to close a venous stasis ulcer. Some cases require a procedure to improve blood flow in deep veins of the legs, using angioplasty and/or stents.
Ultimately, the goal of our recommended therapy is to increase venous return from the legs (push blood back up the leg), thereby decreasing symptoms associated with vein disease and preventing further venous disease progression.
Our doctors are vascular and vein experts, providing you with the safest choice for successful treatment of vein disease.
Call 832-886-0137 today to schedule your appointment.






